Case
72 Diagnosis |
Versión
en Español |
|||
Go back to clinical information and images
Diagnosis: AA amyloidosis (secondary amyloidosis)
Staining for Congo red was positive (Figures 12 and 13). Immunostaining for AA amyloid was also positive (Figures 14 and 15). The final histologic diagnosis was AA (secondary) amyloidosis, associated to psoriasis.

Figure 12. Congo red staining. Right with polarized light. X400.

Figure 13. Congo red staining. Right with polarized light. X400.
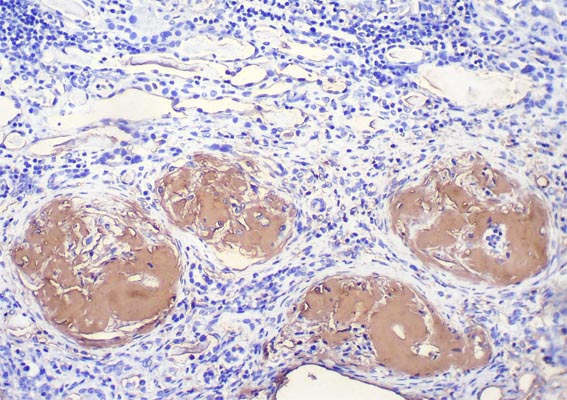
Figure 14. Immunostaining for A amyloid (AA), X400.

Figure 15. Immunostaining for A amyloid (AA), X400.
Amyloid A (AA) amyloidosis (also referred as "secondary amyloidosis") is the most common form of systemic amyloidosis worldwide. It is characterized by extracellular tissue deposition of fibrils that are composed of fragments of serum amyloid A (SAA) protein, a major acute-phase reactant protein, produced predominantly by hepatocytes. AA amyloidosis occurs in the course of a chronic inflammatory disease of either infectious or noninfectious etiology, and with certain neoplasms such as Hodgkin disease and renal cell carcinoma. In developing countries, the most common instigator of AA amyloidosis is chronic infection; in industrialized societies, rheumatic diseases, such as rheumatoid arthritis (RA), are the usual stimuli. The tissue fibril consists of a 7500-dalton cleavage product of the SAA protein, which is an acute phase reactant, and like C-reactive protein, is synthesized by hepatocytes under the transcriptional regulation of cytokines including interleukin (IL)-1, IL-6 and tumor necrosis factor (TNF). Several lines of evidence have indicated that the conversion of SAA into amyloid fibrils occurs through its specific interaction with heparan sulphate, a ubiquitously expressed glycosaminoglycan component of the extracellular matrix. SAA specifically binds to heparan sulfate (HS) glycosaminoglycan, a common constituent of all types of amyloid deposits that has been shown to facilitate conformational transition of a precursor to beta-pleated sheet structure. (El anterior texto fue tomado de: Dhawasn R et al. AA (Inflammatory) Amyloidosis. In eMedicine. Consulted 27th February, 2012. Link: http://emedicine.medscape.com/article/335559-overview).
Morphologically primary (AL) and secondary (AA) amyloidosis are indistinguishable. Molecular studies are needed to differentiate these diseases.
See the chapter: Amyloidosis, multiple myeloma... of our tutorial.
Go back to clinical information and images
References
-
Girnius S, Dember L, Doros G, Skinner M. The changing face of AA amyloidosis: a single center experience. Amyloid. 2011 Jun;18 Suppl 1:221-3. [PubMed link]
-
Dhawasn R et al. AA (Inflammatory) Amyloidosis. In eMedicine. Consulted 27th February, 2012. Link: http://emedicine.medscape.com/article/335559-overview
-
van der Hilst JC. Recent insights into the pathogenesis of type AA amyloidosis. ScientificWorldJournal. 2011;11:641-50. [PubMed link] [Free full text link]
-
Picken MM. Amyloidosis-where are we now and where are we heading? Arch Pathol Lab Med. 2010;134(4):545-51. [PubMed link] [Free full text link]
-
Ryan JG, Dorman AM, O'Connell PG. AA amyloidosis in psoriatic arthritis. Ir J Med Sci. 2006;175(2):81-2. [PubMed link]
-
Kagan A, Husza'r M, Frumkin A, Rapoport J. Reversal of nephrotic syndrome due to AA amyloidosis in psoriatic patients on long-term colchicine treatment. Case report and review of the literature. Nephron. 1999;82(4):348-53. [PubMed link]