Case
7 With discussion |
Versión
en Español |
|||
CASE 7
Clinical information
A 49-years-old man with non-histologically classified chronic glomerulonephritis and end-stage renal disease underwent kidney allograft transplantation from cadaveric donor 10 years ago. Allograft function was satisfactory until 5 months ago when in a control review nephrotic range proteinuria (8.3 g/24h) and renal disfunction (serum creatinine: 3.2 mg/dL) were detected. In the urinalysis 5 eritrocites/HPF and several cylinders were found.
Recurrent glomerular disease versus chronic rejection were the diagnosis posibilities for the doctors treating the patient, and a renal biopsy was undertaken.
The patient presented fever and cytopenia. No skin lesions; no heart or lung alterations. ANAs and ANCAs negative; no complement level alterations; serun alanine aminotrasferase: 45 U/L, and aspartate aminotrasferase: 47 U/L. Hepatitis virus tests (B and C) negatives. The patient history was relevant for mild hypertension without other systemic disease. He does not have diabetes.
Due to severe and progressive impairement of kidney function and persistent severe proteinuria, nephrectomy of the allograft was carried out.
What is your clinical diagnosis?
See the images.
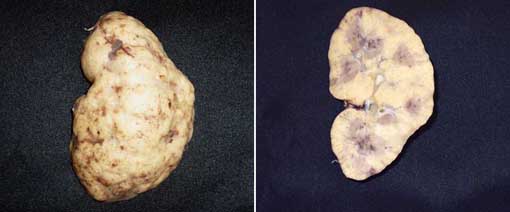
Figure 1. Macroscopic images of the allograft nephrectomy.

Figure 2. Left: H&E, X200; right: H&E, X400.

Figure 3. Left and right: H&E, X400.

Figure 4. Left: H&E, X200; right: H&E, X400.

Figure 5.Left: Masson's trichrome stain, X400; right: PAS, X200.

Figure 6. Left: methenamine silver stain, X400; right: methenamine silver stain, X200.
What is your diagnosis?
Do you like another ancillary
study for a more precise diagnosis?